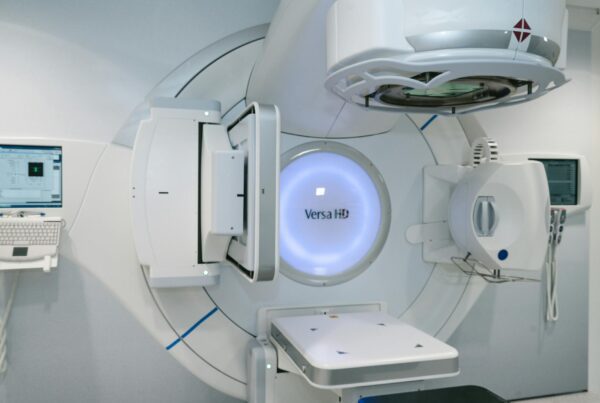
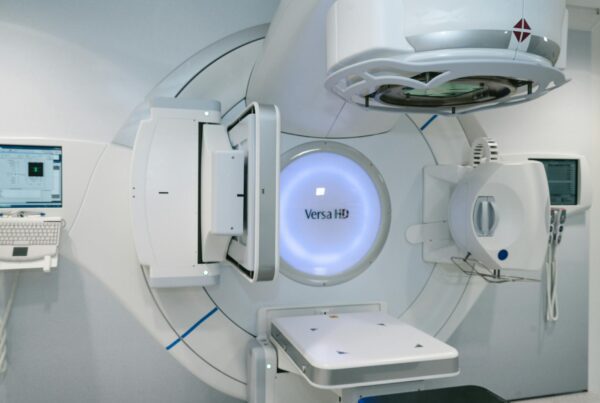
Simulating electron transport in clinical linear accelerators and computing dose distributions in brachytherapy rank among the most demanding challenges in computational medical physics. The Monte Carlo method provides the most accurate tool for solving both, overcoming fundamental limitations of analytical algorithms. In this article, we explore how Monte Carlo modelling has evolved for external electron beams and for brachytherapy source dosimetry — two applications requiring distinct levels of rigour.
Series overview: for the full roadmap and related articles, return to the complete guide on Monte Carlo in radiotherapy.
For a comprehensive overview of all Monte Carlo applications, see our complete guide to Monte Carlo techniques in radiotherapy.
In This Article
- 1. Clinical Electron Beams: Why Monte Carlo Is Essential
- 2. Early Work in Electron Beam Modelling
- 3. Complete LINAC Models for Electron Beams
- 4. The BEAM Code and Electron Beam Applications
- 5. Treatment Planning and Advanced Techniques
- 6. Monte Carlo in Brachytherapy: Fundamentals
- 7. Single-Source Dosimetry and the TG-43 Formalism
- 8. Cross Sections and Dose Estimators
Clinical Electron Beams: Why Monte Carlo Is Essential
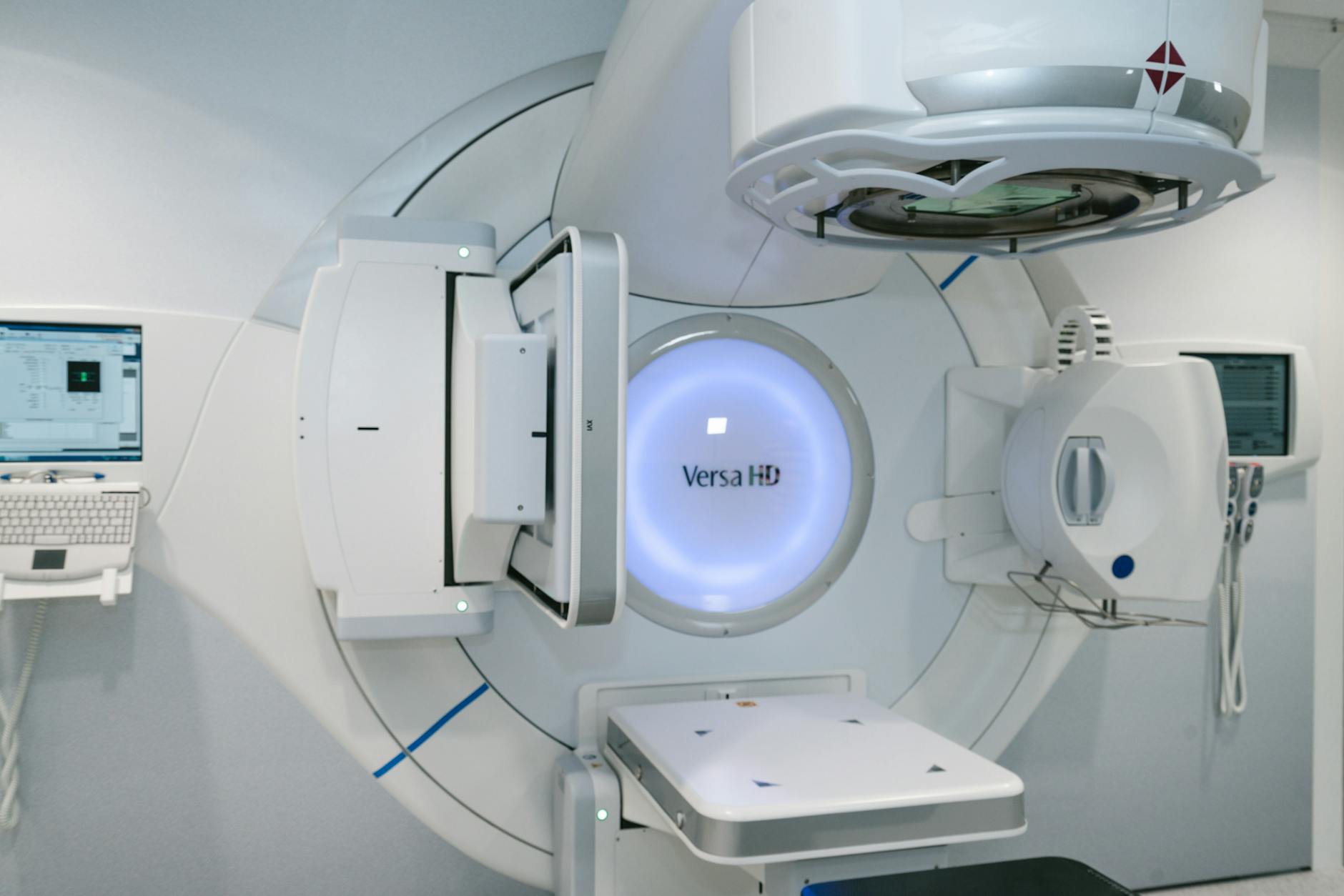
Monte Carlo simulations are indispensable for dose calculation in electron beams — even more so than for photons. The reason is straightforward: analytical dose calculation algorithms for electrons show significant errors in irregular fields and heterogeneous targets, even in modern treatment-planning systems. While alternative methods can rival Monte Carlo accuracy for photons, the situation is different for electrons, with numerous studies exposing flaws in conventional methods.
Clinical electron beams typically use energies ranging from 4 to 20 MeV. The LINAC configuration for electrons differs from photon mode in three key aspects: there is no photon conversion target, a scattering foil broadens the beam, and a multi-stage collimator (applicator) shapes the field close to the patient surface. This proximal collimation is necessary because electrons scatter far more in air than photons.
Early Work in Electron Beam Modelling
Berger and Seltzer, in 1978, were among the first to model the interaction of electrons with lead scattering foils — the LINAC component that most significantly influences the electron beam and where contaminant bremsstrahlung photon production occurs. They found that the intervening air causes significant energy degradation of the electron beam, while the effect of air can be ignored in high-energy photon beams. The same group that pioneered Monte Carlo photon beam modelling was also one of the first to present a Monte Carlo model for a clinical electron beam.
Borrell-Carbonell et al. published simplified LINAC models in 1980, treating beam collimators as apertures with no wall interactions — an approximation that does not yield a realistic particle fluence for electron beams. Rogers and Bielajew (1986) compared calculated and measured depth-dose curves for monoenergetic electrons, noting that simulations predicted a less steep dose gradient near the surface and an excessively steep dose fall-off beyond the depth of maximum dose. Passing electrons through the simulated exit window, scattering foils, and air reduced these differences.
Andreo and Fransson (1989) showed that stopping-power ratios are relatively insensitive to the details of the electron spectrum, but emphasized that preserving the energy–angle correlation is critical — a direct implication for virtual source models. Ebert and collaborators studied simple models of applicators and Cerrobend cutouts, identifying two main processes: electron scatter off the inner edges and bremsstrahlung production.
First Complete LINAC Models for Electron Beams
Modelling electron beams is widely regarded as more difficult than photon beams, owing to the greater sensitivity of particle fluences and absorbed-dose distributions to primary-beam details (energy, spatial, and angular distribution) and LINAC geometry — particularly the scattering foils and applicators.
The pioneering efforts to model complete electron beam geometries with EGS4 were made by Udale and Udale-Smith. Their models for Philips LINACs included the exit window, primary collimator, scattering foils, monitor chamber, mirror, movable photon jaws, accessory ring, and applicator.
Udale simulated five configurations of increasing complexity: from a monoenergetic pencil beam in vacuum to the full LINAC geometry. She used measured depth-dose distributions to tune the primary electron beam energy by matching $R_{50}$ and the practical range $R_p$. Electron range rejection was employed as a variance-reduction technique, avoiding transport of electrons that could not reach the LINAC exit. She scored phase-space files at the bottom of the LINAC and, in a second step, used these for phantom dose calculations. She also demonstrated that some degree of correlation between position, energy, and angle must be maintained to avoid loss of simulation accuracy.
Udale-Smith compared models of several LINACs and established that some had superior designs: fewer contaminant photons, lower-energy contaminant photons, fewer scattered electrons, and narrower angular distributions. Monte Carlo simulation is the ideal tool for such comparative equipment-design studies.
The BEAM Code and Electron Beam Applications
The advent of the BEAM code in 1995 was a landmark in Monte Carlo modelling of LINACs, including electron beams. In fact, most early results reported with BEAM were for electron beams. The code provides a wide array of geometry modules, source geometries, variance-reduction techniques, scoring techniques, and tagging methods.
The original 1995 paper by Rogers et al. demonstrated excellent agreement between measured and simulated dose distributions for a 20 MeV beam from a research LINAC with very well-known characteristics. In clinical practice, the necessary LINAC details are often unavailable, forcing users to “tune” the model.
Ma et al. investigated multiple source models exploiting virtual point-source positions due to the diffusivity of electron scatter — making source model derivation more complicated for electrons than for photons. Verhaegen et al. studied backscatter to the monitor chamber: the relative signal increase was 2% when jaws decreased from 40 cm to 0 cm in a 6 MeV beam, smaller for higher energies. Notably, in electron beams, the spectral shape differs significantly between forward and backscattered electrons.
Determining the electron spot size on the scattering foils is critical. Huang et al. (2005) derived FWHM values of 1.7–2.2 mm for 6–16 MeV beams and noted a primary beam shift of up to 8 mm from the LINAC centre. Primary electron beam information remains among the hardest to estimate clinically.
Treatment Planning and Advanced Techniques
Conventional electron treatment-planning systems have well-documented errors in irregular fields and heterogeneous targets. Monte Carlo algorithms offer unparalleled accuracy. Fast MC codes for electron treatment planning were introduced by Neuenschwander et al. (MMC, 1995) and Kawrakow et al. (VMC, 1996). Ma and collaborators addressed clinical beam simulation, beam characterisation, air-gap factors, commissioning procedures, and stopping-power ratios.
Modulated electron radiation therapy (MERT) was extensively studied by Ma et al. Al-Yahya et al. designed a few-leaf electron collimator using Monte Carlo during the design stage. The full range of deliverable rectangular fields, combined with available electron energies, fed an inverse-planning algorithm based on simulated annealing. The authors showed that highly conformal treatments can be planned this way.
A noteworthy recent development is FLASH radiotherapy, exploiting ultra-high dose rates to create differential biological response between tumour and normal tissue. Lansonneur et al. conducted one of the few studies using Monte Carlo simulations with the GATE code for FLASH electron radiotherapy. For foundational concepts, see our article on Monte Carlo fundamentals in radiotherapy.
Monte Carlo in Brachytherapy: Fundamentals and Evolution
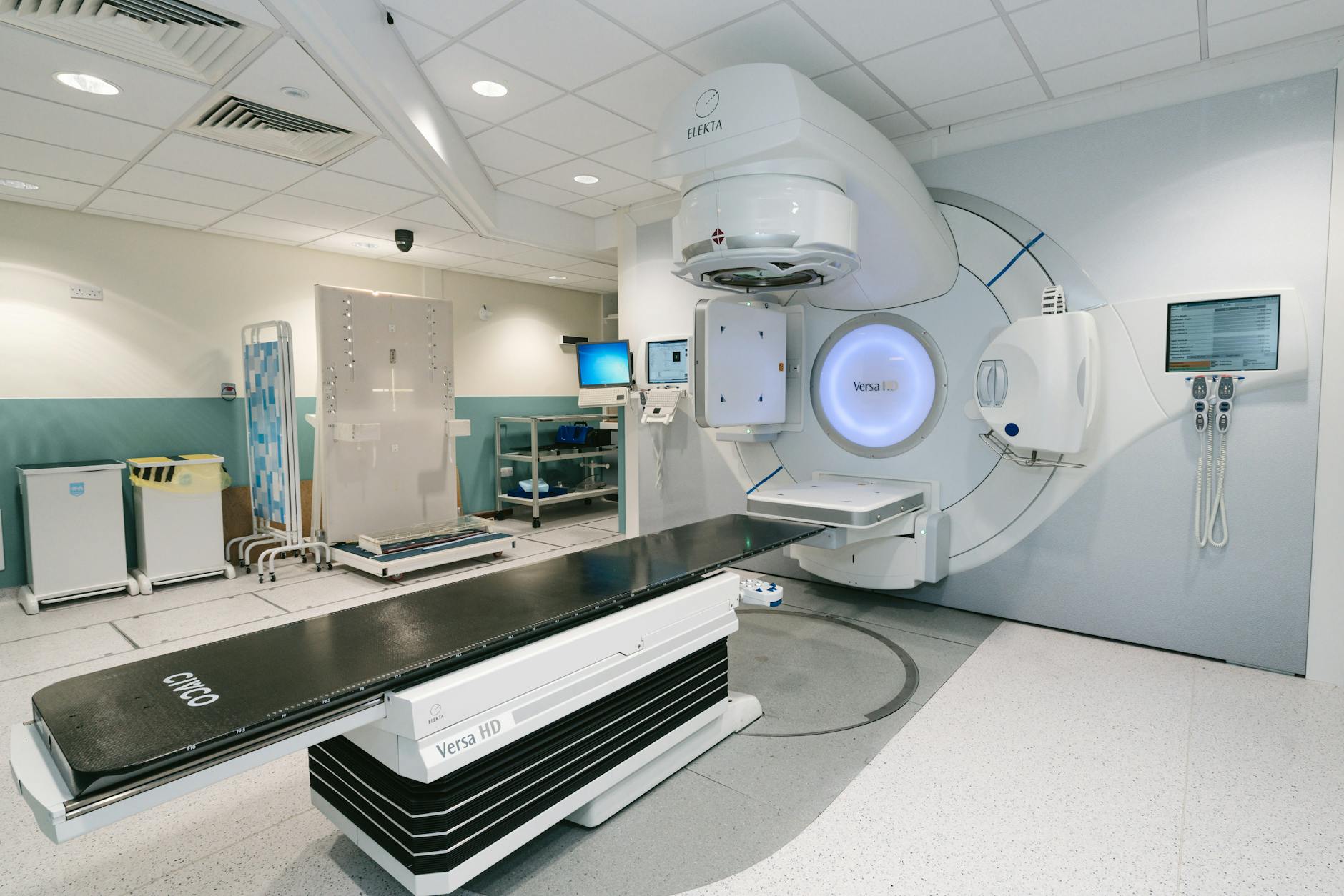
In brachytherapy (BT), Monte Carlo simulation has become an essential dosimetry tool, playing key roles in both clinical practice and research. The most established application is the determination of dose-rate distributions around individual sources. Modern sources contain low-energy radionuclides (mean energies < 50 keV) such as $^{103}$Pd, $^{125}$I, or $^{131}$Cs; higher-energy radionuclides such as $^{192}$Ir, $^{137}$Cs, or $^{60}$Co (mean energies of 355, 662, or 1,250 keV); or miniature X-ray sources.
In low-dose-rate (LDR) BT, radioactive material is encapsulated in permanently implantable seeds. In high-dose-rate (HDR) BT, an iridium pellet is encapsulated and welded to the tip of a remote afterloader cable. While inverse-square-law dependence dominates BT dose distributions, photon attenuation and scatter buildup in the surrounding medium, combined with radiation interactions within the source structure, give rise to anisotropic dose distributions.
The first computational efforts date back to the 1960s, with Meisberger deriving tissue-attenuation factors for $^{198}$Au, $^{192}$Ir, $^{137}$Cs, $^{226}$Ra, and $^{60}$Co point sources. The first 3D MC model of a BT source geometry was performed in 1971 by Krishnaswamy for $^{252}$Cf needles. A landmark: Williamson showed in 1983 that the Sievert integral deviated by 5%–100% from MC results for monoenergetic photons below 300 keV. Burns and Raeside were the first to fully model a commercial $^{125}$I seed (model 6711), including the silver marker, radioactivity distribution, and titanium encapsulation.
Single-Source Dosimetry and the TG-43 Formalism
The rising popularity of LDR prostate seed implantation in the US — from 5,000 in 1995 to about 50,000 in 2002 — fuelled growth in commercially available BT seeds. The original TG-43 report (1995) presented consensus dosimetry parameters for one $^{103}$Pd and two $^{125}$I seeds. The TG-43U1 update (2004) covered 8 models; the 2007 supplement added 8 more; and the 2017 supplement addressed remaining commercial low-energy sources.
The TG-43 formalism requires dosimetry data extracted from MC-computed or experimentally measured dose distributions. Key parameters include the dose-rate constant $\Lambda$, the radial dose function $g_L(r)$, and the 2D anisotropy function $F(r,\theta)$. The AAPM prerequisite that at least one experimental and one MC determination be published before clinical use made MC simulations a de facto dosimetry standard.
An important caution: MC results should not be trusted blindly. Significant dose-estimation differences arise from different photon-interaction cross-section databases. In the < 50 keV range, where photoelectric absorption dominates, 1%–2% cross-section errors can produce 10%–15% dose errors at 5 cm from a seed. This led to the adoption of modern cross-section libraries derived from theoretical quantum-mechanical models.
Cross Sections and Dose Estimators
Cross-section library selection is critical for MC simulations in brachytherapy. Modern libraries — EPDL97, DLC-146, and XCOM — share the same theoretical foundations despite format differences. For BT, accurate post-1983 photoelectric and scattering cross sections are essential.
Omitting electron transport and simulating only photon transport substantially reduces the computational burden. This simplification — approximating absorbed dose by collision kerma — is valid everywhere for low-energy sources (electron ranges < 0.1 mm). For high-energy sources ($^{192}$Ir, $^{137}$Cs, $^{60}$Co), with secondary electron ranges of 1–5 mm, the charged-particle equilibrium approximation may introduce significant errors near metal-tissue interfaces. Dose errors exceeding 15% at distances less than 1 mm from an HDR $^{192}$Ir source have been reported.
The track-length estimator offers dramatic efficiency gains over the analogue estimator: factors of 20–50 for $^{125}$I, and up to 70 ($^{103}$Pd), 90 ($^{125}$I), and 300 ($^{192}$Ir) for different BT treatments. For more on photon beam modelling foundations, consult our article on Monte Carlo modelling of external photon beams.
Outlook and Final Remarks
Monte Carlo simulations are powerful and increasingly essential tools in electron beam radiotherapy and brachytherapy. For electrons, the advantage over analytical algorithms is even more pronounced than for photons. MC plays a decisive role in designing complex delivery techniques such as MERT and, more recently, FLASH radiotherapy.
In brachytherapy, Monte Carlo has been consolidated as the standard for individual source dosimetry, underpinning the TG-43 formalism that forms the basis of clinical practice. MC methodology, extensively benchmarked against experimental measurements with 1%–3% accuracy, is mature and robust enough to support clinical dosimetry across the entire BT energy spectrum.
EGS/EGSnrc-based codes (including the BEAM user interface) have historically dominated this field, but GEANT4 is seeing increased use. An important caveat: since MC codes generally differ more in cross sections and transport methods for electrons than for photons, rigorous benchmarking is essential for electron beam simulations.