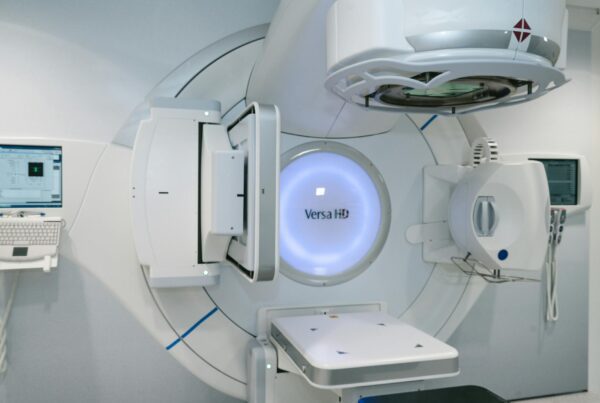
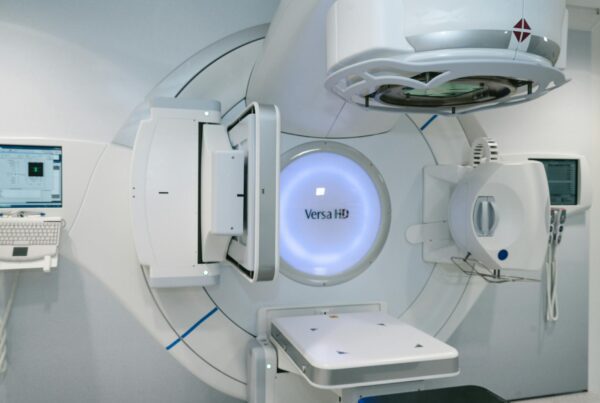
What Is Dynamic Beam Delivery and Why Monte Carlo Matters
Dynamic delivery techniques — IMRT, tomotherapy, and VMAT — are now routine in radiotherapy clinics worldwide. In these approaches, particle fluence is modulated by beam modifiers such as multileaf collimators (MLCs), whose positions vary continuously during irradiation. Some techniques also change the beam direction and energy simultaneously, as in arc therapy or scanned proton beams.
Series overview: for the full roadmap and related articles, return to the complete guide on Monte Carlo in radiotherapy.
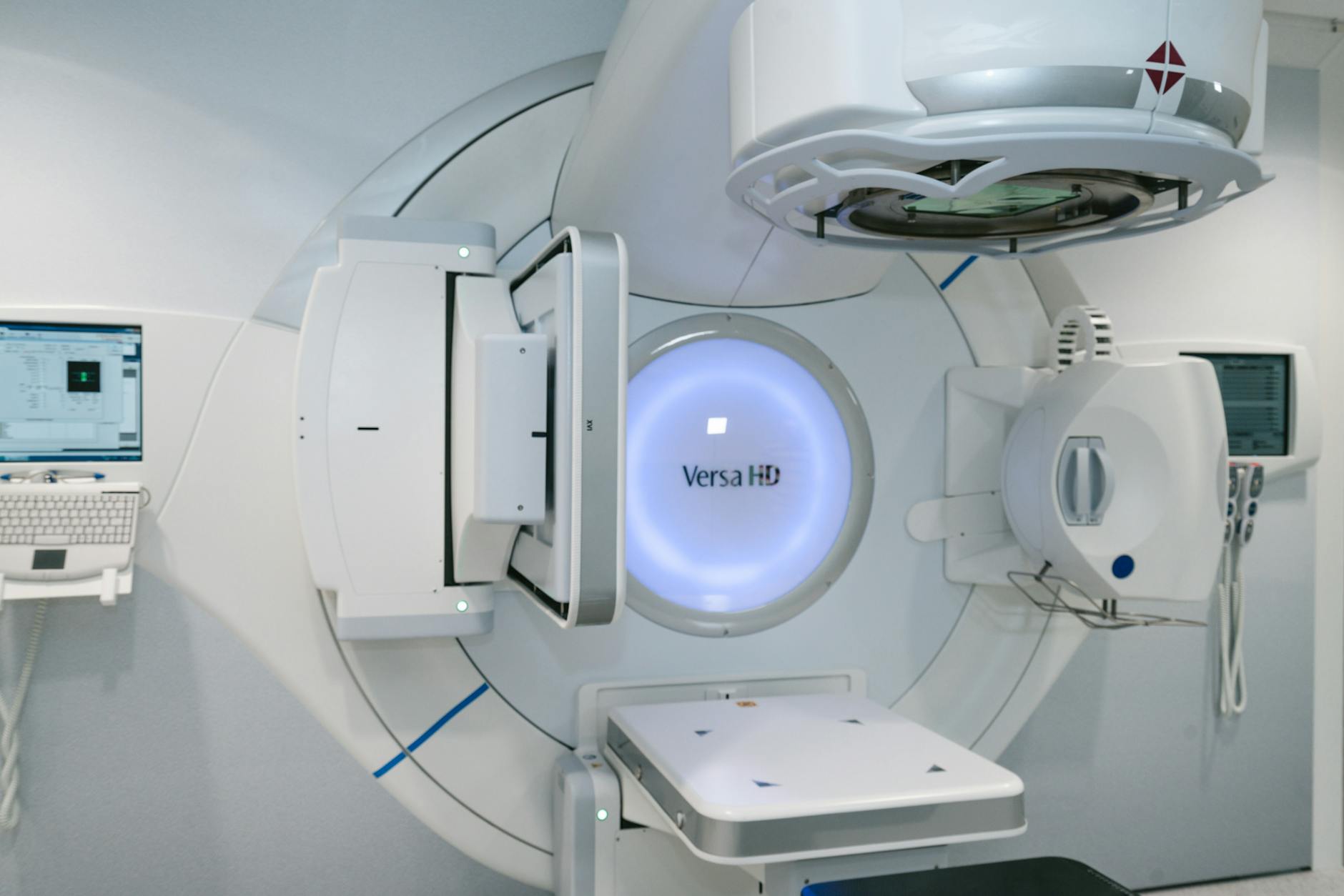
Monte Carlo (MC) simulation provides the dosimetric accuracy needed to characterize these dynamic beam modifiers, verify treatment planning system (TPS) dose distributions, and perform independent monitor unit (MU) calculations. Its superiority in low-density tissue like lung — compared to analytical algorithms — makes MC a natural choice for 4D radiotherapy. A properly validated dynamic MC model can replace extensive measurements during commissioning, especially when measurement resolution or accuracy is questionable. For a broader overview, see our complete guide to Monte Carlo techniques in radiotherapy.
Strategies for Simulating Time-Dependent Beam Geometries
Three main approaches exist for handling dynamic geometries in MC simulations, listed in order of increasing complexity.
Particle weighting uses ray tracing through beam modifier geometry to determine attenuation-based weighting factors. Temporal variations are accounted for by scaling these factors by the fractional delivery time. Ma et al. (2000) applied this to recalculate IMRT treatment plans from the CORVUS TPS. The main limitation is that non-uniform particle weights increase statistical variance — particle splitting and Russian roulette help but add complexity.
The Static Component Simulation (SCS) method runs multiple discrete simulations of individual geometrical states. It works naturally for step-and-shoot IMRT, where geometry changes occur in discrete steps. Importantly, simulating more geometries does not necessarily increase total calculation time since the total number of histories is distributed across individual geometries. The overhead comes from input file preparation, initialization, and post-processing. Shih et al. (2001) used this approach to reproduce Varian dynamic wedge delivery with 20 jaw positions.
The Position-Probability Sampling (PPS) method, developed by Liu et al. (2001), randomizes geometry sampling using cumulative probability distribution functions (CPDFs) that describe the fraction of total delivery time for each configuration. For each incident particle history, the MLC position is randomly sampled from this CPDF. In practice, PPS tends to be more operationally efficient than SCS, and both approaches produce the same statistical variance for an equal number of incident particles.
Dynamic Wedge and MLC-Based IMRT Applications
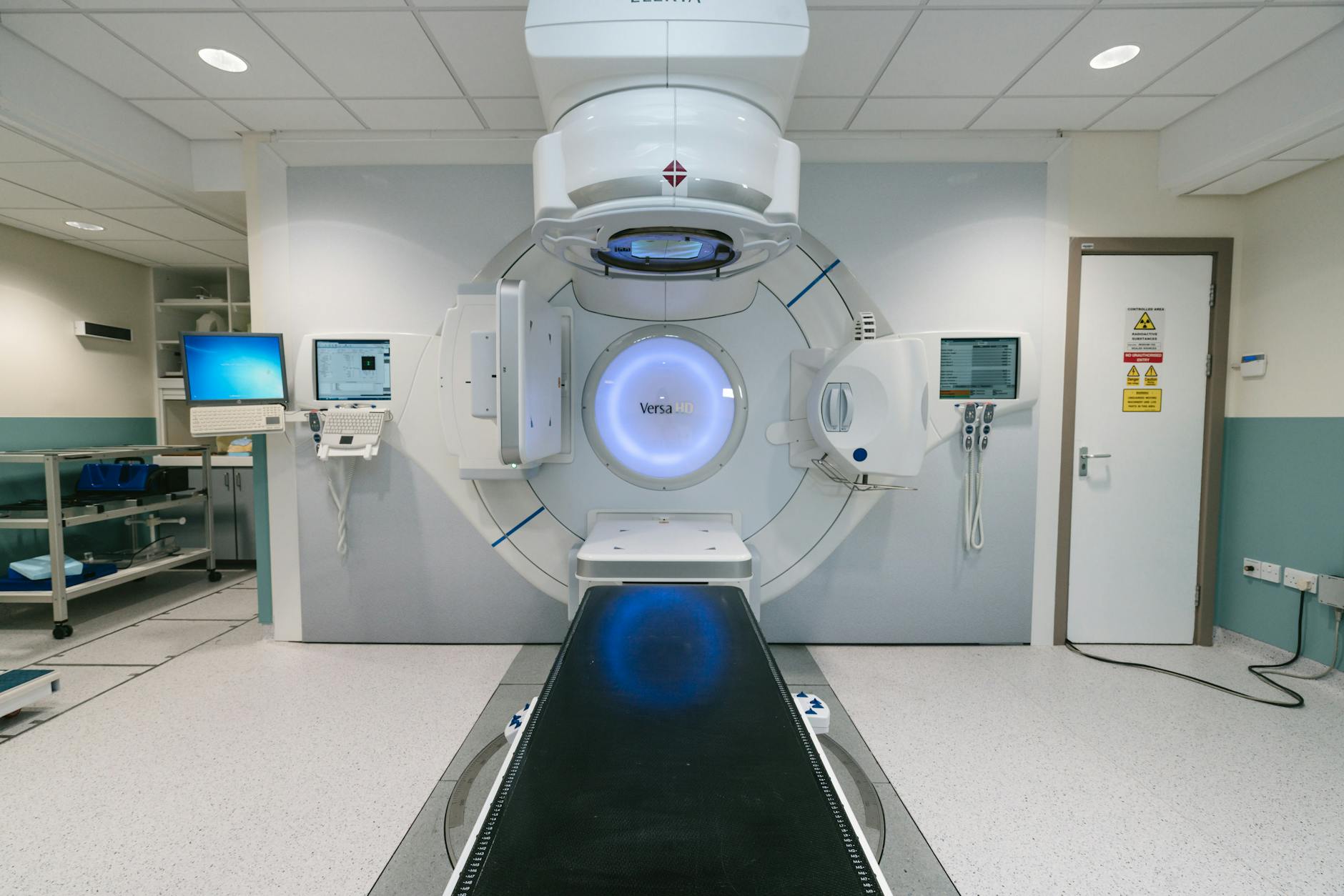
The first reported MC simulation of a dynamic wedge was performed by Verhaegen and Das (1999) using EGS4/BEAM on a Siemens linac. They modeled wedge angles from 15° to 60° for energies of 6–10 MV, obtaining good agreement with measurements except in the penumbra region of the wedge toe end (discrepancies up to 4%). No major differences were found between physical and virtual wedges for beam hardening effects, except that 60° physical wedges produce significantly harder beams due to higher tungsten absorption.
For MLC-based IMRT, Deng et al. (2001) demonstrated that intensity maps calculated with a ray-tracing algorithm that includes tongue-and-groove geometry differ significantly from simplified maps — an important finding for dose accuracy. The fast MC code VCU-MLC (Siebers et al., 2002) uses a single-Compton approximation for photon interactions within the MLC, with no electron transport. Each incident particle’s weight is modified by randomly sampling 100 MLC positions from the leaf sequence file and averaging transmission probabilities, providing substantial efficiency gains.
Leal et al. (2003) and Seco et al. (2005) performed the first complete linac-to-patient simulations for Siemens and Elekta linacs using BEAMnrc, with 5–15 segments per beam and histories proportional to segment MUs. For more detail on photon beam modeling, see our article on Monte Carlo modeling of external photon beams.
Tomotherapy and VMAT: Continuous Gantry Rotation
Simulating tomotherapy and VMAT is especially challenging because the gantry angle changes continuously. Helical tomotherapy uses a rotating fan beam with binary MLC modulation, specified by a sinogram file with fractional opening times at discrete gantry positions.
Sterpin et al. (2008) developed TomoPen, a PENELOPE-based user code, subdividing each sinogram entry into 11 subprojections with linearly interpolated leaf openings. Comparison with film and ionization chamber measurements showed agreement within 2% and 1 mm. Zhao et al. (2008a) took a different approach with EGSnrc/BEAMnrc, using the SCS method with the VARMLC component module for each subprojection.
For VMAT, Bush et al. (2008) modeled Varian RapidArc delivery using EGSnrc/BEAMnrc. They addressed the significant leaf motion between gantry control points by calculating a mean gantry angle for each consecutive pair of positions and using the adjacent leaf openings as control points for a DMLC delivery at that mean angle. Variable dose rate is accounted for by weighting the dose calculation by fractional MUs.
Two PPS-based approaches for BEAMnrc were developed by Lobo and Popescu (2010) using ISOURCE 20/21 in DOSXYZnrc, where each particle is “time-stamped” with a randomly sampled fractional MU index that synchronizes all dynamic components — jaws, MLC, gantry rotation, collimator, and couch translation.
Dynamic Patient Simulations: Respiratory Motion
The need for 4D patient dose calculation arose from interest in compensating for respiratory motion effects (Keall et al. 2004). Bortfeld et al. (2004) identified three motion effects on delivered dose: (1) blurring along the motion path, (2) localized spatial deformations at organ boundaries with density changes, and (3) interplay between tumor motion and dynamic beam delivery.
For those interested in the Monte Carlo fundamentals underlying these calculations, see our article on Monte Carlo fundamentals in radiotherapy.
Convolution-Based Methods
The simplest approach convolves the dose distribution with a probability distribution describing positional variations (Lujan et al., 1999). This models only the blurring effect, ignoring differential deformations. The spatial invariance assumption breaks down at tissue interfaces, leading to dose underestimation at these locations.
Dose-Mapping Methods: Center-of-Mass and Interpolation
The center-of-mass (COM) remapping method uses deformable image registration to map doses between respiratory phases. Paganetti et al. (2004) implemented COM in GEANT4, updating patient geometry across 10 breathing phases from a 4D-CT dataset. Trilinear interpolation improves upon COM by considering neighboring voxels, but Heath and Seuntjens (2006) showed that interpolation errors cause incorrect dose calculations in regions of large dose and deformation gradients.
Voxel Warping: Energy Conservation
Heath et al. (2007) developed defDOSXYZnrc, which deforms reference dose grid voxels using displacement vectors from deformable image registration. Densities are adjusted according to volume changes to conserve mass. The Jacobian determinant identifies transformation discontinuities:
$$\det J(N(x)) = \begin{vmatrix} \frac{\partial u_x}{\partial x} + 1 & \frac{\partial u_x}{\partial y} & \frac{\partial u_x}{\partial z} \\ \frac{\partial u_y}{\partial x} & \frac{\partial u_y}{\partial y} + 1 & \frac{\partial u_y}{\partial z} \\ \frac{\partial u_z}{\partial x} & \frac{\partial u_z}{\partial y} & \frac{\partial u_z}{\partial z} + 1 \end{vmatrix}$$
Where $u_x$, $u_y$, $u_z$ are the displacement field components. A negative determinant at a node indicates a discontinuity in the transformation.
The VMC++ reimplementation (Heath and Kawrakow, 2011) achieved a 130-fold improvement in computational efficiency using optimized tetrahedral geometry elements — each deformed voxel divided into 6 tetrahedra.
Interplay Effects and Combined Dynamic Simulations
The interplay effect — the interaction between MLC leaf motion and tumor movement — is a central concern in intensity-modulated radiotherapy. Yu et al. (1998) showed that dynamic collimation causes large local photon dose errors per fraction due to motion in the beam penumbra region. The magnitude depends strongly on beam aperture speed relative to target motion speed and beam width relative to motion amplitude.
For proton beams, interplay effects involve additional factors: (1) patient breathing, (2) energy change times, (3) motion amplitude, and (4) the rescanning methodology used (Seco et al., 2009a).
Gholampourkashi et al. (2017) combined ISOURCE 21 with voxel warping in 4DdefDOSXYZnrc, creating a comprehensive 4D MC simulation tool. For each incident particle, the MU index that samples dynamic collimator settings also determines the fractional breathing amplitude from a normalized respiratory trace. Validation was performed with film and MOSFET measurements in a programmable deformable lung phantom (Gholampourkashi et al. 2020).
Future Applications of MC in Dynamic Beam Delivery
The 4D MC methods summarized here can simulate deliveries with far more degrees of freedom than conventional linacs allow. Such deliveries are already possible with Developer Mode TrueBeam linacs (Varian), CyberKnife, and Vero-SBRT systems — but no commercial TPS can currently calculate dose for trajectories of such complexity.
| Approach | Method | Best Application | Main Limitation |
|---|---|---|---|
| Particle Weighting | Ray tracing + weight factors | Fast calculations, simple IMRT | High statistical variance |
| SCS (Static Component Simulation) | Multiple discrete static simulations | Step-and-shoot IMRT | I/O and post-processing overhead |
| PPS (Position-Probability Sampling) | Random CPDF sampling | VMAT, tomotherapy, continuous geometries | Implementation complexity |
| VCU-MLC | Single Compton + 100-sample averaging | IMRT with optimized efficiency | Simplified transport physics |
| Voxel Warping (VMC++) | Deformable tetrahedral geometry | 4D patient simulations | Requires continuous deformation field |
| EMCM | Energy and mass congruent mapping | Dose accumulation with mass conservation | 100-subvoxel subdivision |
Source: Monte Carlo Techniques in Radiation Therapy (2nd ed., CRC Press, 2022)
The future points toward using these 4D MC tools for both verification and planning of treatments with increasing degrees of freedom — including continuous collimator rotation, couch translation, and real-time adaptation. For insights on how Monte Carlo applies to proton beams, see our article on ion beam and device design with Monte Carlo.