What Is RIS in Radiology?
Radiology Information System (RIS) is the generic name for an application or group of applications used to handle textual data related to imaging procedures, such as examination details, attendance lists, appointment schedules, reports, and billing data.
It also includes data such as radiation dose and operator details, and stores any medications prescribed or administered solely as part of the imaging examination — for instance, contrast in IVU (intravenous urography) or glyceryl trinitrate in CT imaging.
Predominantly a text-based application (with scanned paper forms also available in many cases), the earliest RIS systems were simply created to replace the paper appointment books widely used at the time. They became necessary as workloads increased, the types of examinations offered expanded, and departments grew to a point where it became impractical to continue using a single logbook to track multiple rooms with very different scheduling lengths.
Example of a Radiology RIS System
From a technology standpoint, much like the image output of radiological examinations, the textual data generated within a department is also structured. This lends itself to being placed in a tabular database structure, with individual components of a selected entry placed on screen in the appropriate positions. However, since the vast majority of data handled by a RIS is text, the scale and hardware required to operate the application are significantly smaller.
By their very nature, RIS systems are exclusive to Radiology. Other departments have similar systems tailored to their textual workflows, known generically as Clinical Information Systems (CIS). For example, Pathology uses a LIS (Laboratory Information Management System). When choosing a RIS for your hospital or clinic, it is important to consider the following key points:
Integration: Ensure that the RIS integrates seamlessly with existing systems, such as PACS and EHRs, to reduce manual data entry and improve accuracy.
Ease of Use: A RIS should be user-friendly and easy to navigate, with an intuitive interface and customizable settings.
Security and Compliance: Make sure the RIS complies with all applicable regulations, including HIPAA and HL7, and has robust security measures in place to protect patient data.
Reporting and Analytics: The RIS should have robust reporting and analytics capabilities to provide actionable insights into workflow performance, resource utilization, and patient outcomes.
Scalability: The RIS should scale to accommodate practice growth, as well as offer customizable features to meet unique needs.
Support and Maintenance: Look for a RIS provider with a strong track record of customer support and software updates, to ensure the system remains current and effective over time.
By carefully considering these key points, physicians can choose a RIS that will help improve workflow, increase efficiency, and deliver better patient outcomes.
Key RIS Terminology
Accession Numbers
An accession number is a unique identifier assigned to studies, typically allocated by the RIS within the Radiology department. It is sent via a worklist to the modality and passed from both the RIS (to create a folder) and the modality (as part of the images) to the PACS for storage. Accession numbers are typically sequential and, at NHS sites, are in most cases prefixed with the hospital’s national Organization Data Service (ODS) code to help keep them nationally unique — a useful feature when sharing images.
Medical Image Viewer
Examination ID
The use of examination IDs varies depending on the RIS vendor. Many RIS vendors use a sequential number assigned to each examination that is part of the same visit (for example, a visit may include left and right hand — two examinations — each with the same accession number but with 01 and 02 as the examination IDs).
However, some vendors opt to use a permanently fixed examination ID of 0 or 00, preferring to vary the accession number in those cases instead. This lack of standardization sometimes complicates reporting processes when data is shared between hospitals using different RIS vendors.
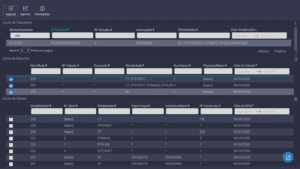
Examination list from a PACS system
SNOMED-CT
The Systematized Nomenclature of Medicine — Clinical Terms (SNOMED-CT) is intended to be a pan-organizational, standard healthcare terminology list that covers all clinical disciplines and is essentially an internationally recognized vocabulary. It is not currently widely adopted in radiology, but it has the potential to provide greater detail about procedures and interoperate with broader parts of a healthcare organization’s informatics environment (particularly with other systems outside of radiology). SNOMED-CT is a product marketed by the International Health Terminology Standards Development Organisation. The use of SNOMED-CT will enable more detailed recording in future Electronic Health Records (EHRs), as improved data coding will allow greater use of machine-based processing, including health prediction algorithms and automated follow-ups.
ODS (NACS)
Another national code list, the ODS list (still commonly known by its former name, the National Administrative Code Service or NACS) provides a list of abbreviations to identify each healthcare provider in the UK. For example, these abbreviations take the form of RT3 (Royal Brompton and Harefield NHS Foundation Trust), RV8 (London North West Healthcare NHS Trust), and RTX (University Hospitals of Morecambe Bay NHS Foundation Trust). They should be used to prefix all generated accession numbers, local room identifiers, and imaging workstation AETs to enable easy identification by external sites (for example, after a data transfer). Originally, the naming of imaging workstation identifiers was left to the discretion of the installing engineer, resulting in hundreds of A&E Room 1s across the country.