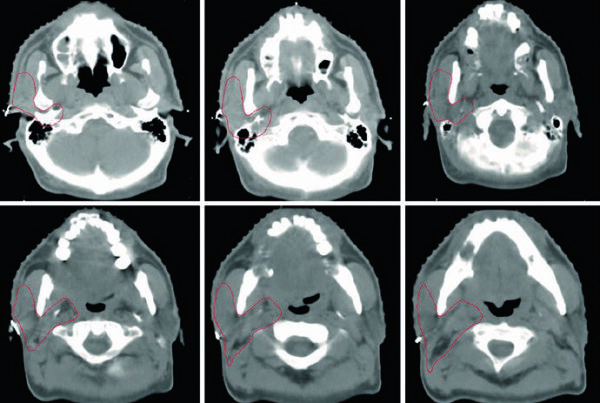
Radiotherapy equipment technical specifications are not just a procurement checklist. When you are setting up a service, they have to translate into import documentation, warranty terms, acceptance testing, maintenance planning, facility readiness, and a safety and quality framework that actually works in day-to-day care.
This dedicated article summarizes what the WHO/IAEA document highlights about building a safe and sustainable radiotherapy service. It is part of our Radiotherapy equipment: technical specifications guide.
Before procurement: documents, import clearance, and device registration
If you want to avoid delays at customs, the work starts as soon as a tender is awarded. The purchaser is expected to obtain key information and documentation in advance to enable an efficient clearance process.
- delivery date;
- copy of the certificate of origin;
- copy of the certificate of conformity;
- commercial invoice;
- final transportation documents (waybill).
Regulatory reality matters too. The text notes that countries with limited historical regulation of medical devices are increasingly implementing requirements, and importation may depend on registration of both the manufacturer and the specific make and model. Where a registered product/manufacturer is missing, an import waiver can often be pursued with the Ministry of Health, but it is typically granted per shipment. That makes early manufacturer engagement essential, because local registration for future procurements can take one to three years in some settings.
Warranty, acceptance testing, and applications training
Clear warranty language and a robust acceptance process protect clinical performance, not just delivery. During procurement, warranties should be requested and the purchaser defines the duration, with a recommendation that the warranty be at least one year.
The warranty is expected to include preventive maintenance, updates and upgrades, spare parts, and labour. The warranty period starts at the end of acceptance testing. Bidders’ maintenance contract terms and conditions for the post-warranty phase are also useful during evaluation so that life cycle costing can be considered.
For major equipment, the specification should define acceptance as testing by the contractor and the end-user (medical physicist) to confirm performance meets the manufacturer’s specifications and the procurement specification. Acceptance test results should be documented and signed by the end-user. Specifications should also state the language for user manuals and maintenance manuals, as well as operation and safety markings.
Manufacturers are expected to demonstrate compliance with ISO standards for good manufacturing practice and ISO quality assurance standards (or equivalent). The document also calls for applications training for the main users: radiation therapists, medical physicists, radiation oncologists, and in-house maintenance engineers. Training for radiation therapists is typically on-site near first clinical operation, and comprehensive off-site training at dedicated centres may be included. This applications training is described as complementary to, not a replacement for, formal education programmes.
Facility readiness: utilities, site planning, and radiation protection features
Even the best specifications fail if the room is not ready. The text points out that major equipment such as LINACs and CT scanners requires specific services, including electric power, lighting, and air-conditioning. Depending on the equipment and manufacturer, additional services such as chilled water or compressed air may be needed.
Radiation protection requirements are also part of the preparation: facility access interlocks, lead glass windows, and radiation beam-on lighting are given as examples. The supplier contract should clearly allocate responsibilities between the hospital and the supplier so that premises are ready for installation with all services in place.
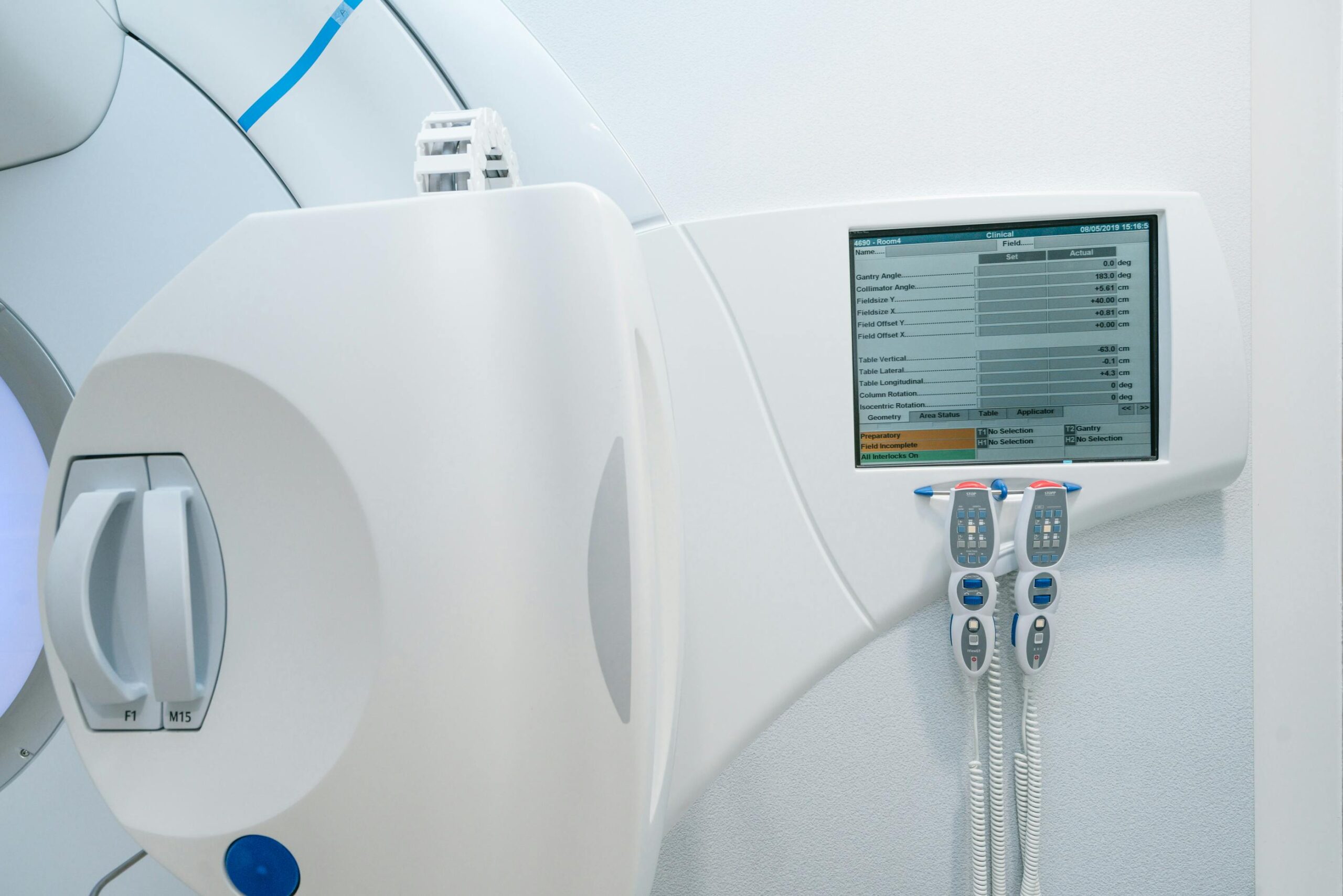
Once the successful bidder is known, consulting the manufacturer’s site planning guide becomes essential. Regular meetings between the hospital implementation team and the supplier, and a pre-installation inspection of the premises, are described as highly recommended. For a broader look at what typically composes a service, see our article on radiotherapy equipment packages.
Radiotherapy equipment technical specifications in maintenance and life cycle planning
Continuity of service after warranty expiry depends on maintenance provisions that are in place for the expected lifetime of major equipment. Maintenance can be delivered through supplier contracts, an in-house engineering service, or a hybrid of both.
When negotiating maintenance contracts, the document lists practical items to address: inclusion of spare parts; inclusion of all safety, hardware, and software updates and upgrades over the lifetime; a regular service schedule (number of service days per year and whether within or outside working hours); help desk access and remote diagnostics; and clarity on whether major parts are included or excluded (for example, the X-ray tube for a CT scanner or the waveguide system for a linear accelerator).
It also suggests checking whether maintenance for locally sourced parts (e.g., UPS, chiller) is included, whether front-line maintenance by trained in-house engineers is included or excluded, and whether contractual penalties are defined. An example is stipulating 95% uptime (available clinical service time as a percentage of normal operating hours) with a penalty of reduced maintenance contract cost in the following year. For corrective maintenance, penalties may also be stipulated for failure to meet a response time (e.g., 24 hours), such as 5% per day of delay of the annual cost.
Maintenance contracts are also recommended for operational software, including TPS and OIS, because they can include software updates and upgrades, help desk access, and hardware fault repair. For equipment-specific specifications in external beam radiotherapy, see radiotherapy equipment technical specifications for EBRT.
Recurring budget items: consumables, licences, and inventory
A safe service needs a budget that accounts for recurring needs. Examples of consumables listed include thermoplastic masks, dressings, and sheets of radiochromic film. Ongoing radiation safety services such as calibrations, renewal of radiation licences, and personal dosimetry services should also be included.
Inventory management of medical devices and equipment is described as essential for continuous delivery. An up-to-date inventory supports budgeting, staffing estimates, contract management, and planning for spare parts and consumables. For ionizing radiation sources, inventories are required by the radiation regulator.
Replacement planning: indicative life cycle durations (Table 19)
Replacement budgeting is tied to expected life cycle durations, but the document cautions that these values are approximate and indicative. Well-maintained equipment may operate safely and effectively for longer or shorter periods depending on usage and environmental conditions. Evidence for replacement includes unreliability with excessive maintenance time, unstable performance, or major damage, and lack of ongoing vendor support for spare parts and service can dictate end-of-life.
For equipment that includes sealed radioactive sources, hospitals need to budget for source exchanges at regular intervals. The cost of replacing a cobalt-60 source for a teletherapy unit can be substantial, and the source exchange contract should include removal and disposal of the old source. At end of life, decommissioning includes safe disposal of radioactive material. The text also notes that a high-energy LINAC may have head activation, and the local radiation regulator should be consulted. Decommissioning costs for sources and equipment should be considered.
Expected life cycle of radiotherapy equipment
The table below reproduces the indicative durations listed in the document.
| Item | Indicative life cycle | Comments |
|---|---|---|
| LINAC | 10–15 years | |
| Cobalt-60 teletherapy unit | minimum 15 years | Including three cobalt-60 source exchanges |
| CT simulator | 5–10 years | |
| Conventional simulator | 10 years | |
| TPS | 5 years | Regular hardware and software updates and upgrades can extend the lifecycle |
| OIS | 5 years | Regular hardware and software updates and upgrades can extend the lifecycle |
| Patient immobilization equipment | 5–10 years | Dependent on usage |
| Mould room equipment | minimum 10 years | |
| Dosimetry, quality assurance (QA) and radiation safety equipment | 10 years | Calibration of radiation detectors at regular intervals is required |
| Superficial/orthovoltage X-ray unit | minimum 15 years | Lifetime could be limited to 10 years depending on the availability of spare parts |
| Brachytherapy afterloader | 10–15 years | Including three cobalt-60 source exchanges |
| Brachytherapy applicators | 3 years | Dependent on usage |
| C-arm fluoroscopic X-ray unit | 10 years | |
| Ultrasound unit | 5–10 years |
Source: Technical specifications of radiotherapy equipment for cancer treatment (Table 19)
Patient safety and quality management: minimum structure
Patient safety is described as paramount in delivering therapeutic radiation doses. The International Basic Safety Standards provide the framework for patient safety and form the basis of legislation and regulations in many countries, complemented by other IAEA safety requirements and an IAEA safety guide for radiation protection and safety in medical uses.
A key principle for therapeutic practice is justification, where the practitioner weighs benefits and detriment of medical exposure. The country’s radiation regulatory body manages the legal and regulatory framework and acts as the contact point for the radiotherapy department on radiation safety and protection. The department appoints a radiation protection officer with a key role in the radiation safety committee representing all staff groups.
Incident reporting and a no-blame learning culture
The incident reporting and learning system is presented as more than a reporting channel: it is a quality, safety, and education tool. Incidents include overdose, underdose, and any geometric miss (right dose in the wrong place). A no-blame culture is encouraged for incident and near-miss reporting, and a nomenclature and reporting framework should be adopted. Learning from incidents often leads to changes in staff practice.
The text points to IAEA SAFRON and the ESTRO ROSEIS platform as examples for further information on incident reporting and learning systems.
Quality management programme: core elements
Quality management is framed as a practical way to deliver high-quality care and, as a result, protect patient safety. Elements include process checks with checklists during treatment planning and treatment (chart check), internal peer review of plans and prescriptions (chart round), and double checks by different staff groups.
It also includes QA on major equipment by establishing baselines and action levels and performing routine quality control tests, and using a quality management committee to implement continuous quality improvement through activities such as process optimization. Based on risk assessment, the programme should also include a QA framework for new techniques and technology.
Independent peer review or audit is presented as a key robustness element, with IAEA offering an audit framework covering clinical and technical aspects. For consistency of national practice, the text recommends common guidelines for nomenclature and reporting, and it points to ICRU reports as a common approach to prescribing, recording, and reporting radiotherapy. Clinical protocols should be evidence-based and aligned with available technology; protocols from clinical trials and the QUANTEC recommendations are cited as pertinent sources, including dose limits for organs at risk.
Education and training: staffing for safe practice
Safe practice requires applications training for relevant professionals, but also comprehensive academic education and clinical training leading to qualification and certification. The document describes principal health professionals required for safe and effective radiotherapy practice, their roles, and recommended education and training requirements.
Principal health professionals in radiotherapy practice (Table 20)
The table below reproduces the roles and training requirements presented.
| Health professional | Definition and role | Education and training | Relevant IAEA publications |
|---|---|---|---|
| Radiation oncologist | A clinical physician with knowledge concerning the causes, prevention and treatment of cancer and other diseases involving expertise in the therapeutic applications of ionizing radiation. | Degree in medicine; at least three years specialty training in radiation oncology. | Syllabus for the education and training of radiation oncologists, Training Course Series No 36, 2012. |
| Medical physicist | A health professional with specialist education and training in the concepts and techniques of applying physics in medicine, competent to practise independently in radiotherapy medical physics. Responsibilities include equipment commissioning, radiation safety and protection, radiation dosimetry, dose optimization and quality management. | Degree in physical sciences or engineering; postgraduate academic degree in medical physics; two to three years of structured clinical training in a radiotherapy department under clinical supervision of a clinically qualified medical physicist. | Roles and responsibilities, and education and training requirements for clinically qualified medical physicists, Human Health Series No 25, 2013; Postgraduate medical physics academic programmes, Training Course Series No 56, 2013; Clinical training of medical physicists specializing in radiation oncology, Training Course Series No 37, 2009. |
| Radiation therapist (RTT) | A technologist with direct responsibility for the daily administration of radiotherapy to cancer patients. | Degree in radiation therapy, including at least one year of clinical training. | A handbook for the education of radiation therapists (RTTs), Training Course Series No 58, 2014. |
| Radiation oncology nurse | A registered professional nurse with responsibilities in care support to patients receiving radiotherapy. | Degree in nursing; subsequent clinical training in radiation oncology of at least 12–16 weeks duration under the direct supervision of a coordinator. | A syllabus for the education and training of radiation oncology nurses, Training Course Series No 28, 2009. |
Source: Technical specifications of radiotherapy equipment for cancer treatment (Table 20)
The text adds that national registration typically accompanies each specialty, implying adherence to a professional code of conduct and requiring ongoing professional development activities to maintain registration. Supporting professions are also listed, including biomedical and maintenance engineers, information technology professionals, social workers, dieticians, physiotherapists, dental surgeons, speech therapists, and administrative staff.
To navigate the series, see the contents overview and return to the full guide for the broader context.